A NICU admission does not mean breastfeeding is impossible! There are many steps you can take to maximize your potential of a successful breastfeeding relationship.
1. Milk expression should begin within 1-6 hours after birth. Within the first hour is ideal. Milk expression should take place with a hospital grade electric breast pump when feeding directly at breast isn’t possible.
Although many pumps are marketed as “hospital grade” they aren’t quite up to par with an actual hospital grade pump like a Medela Symphony. (Your OB can write a prescription for this specific pump so insurance will cover the pump rental from a medical supply shop. This way even when you are no longer at the hospital you are still able to have access to these powerful pumps which are designed specifically to establish and maintain a milk supply!)
2. Current research on pumping & hand expression found that HIGHER milk volumes were obtained when breasts were massaged & warmed prior to pumping, when appropriate breast shield sizes were used, when pumping was initiated within 1 hour of delivery for very low birth weight infants, and frequency increased.
3. Current recommendations are to pump 8-10 times in a 24 hour period ALONG with hand expression in the first 3 days. After the first 3 days pumping should STILL continue to happen at least 8-10 times in a 24 hour period…including throughout the night. If infant is on a 3,6,9,12 feeding schedule in NICU pumping should match that same schedule as infant feeding.
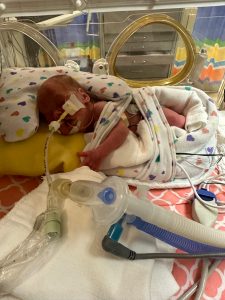
4. If you delivered early milk supply will likely be delayed and take longer. This doesn’t mean you aren’t able to make milk or have low supply! Pumping will stimulate production & trigger the hormone cascade which needs to take place for milk production to happen…although it may take time to see higher volumes of milk it will happen! Even drops of breastmilk can be drawn into a syringe and fed to your infant. Those tiny drops provide HUGE benefits to your infants growing body.
5. Timing for the parent to begin feeding directly at breast is dependent on infant’s signs of
stability. NOT postnatal age or infants current weight.
6. When awaiting the transition of feeding infant directly at breast skin to skin is an excellent way to continue to promote bonding & breastfeeding.
7. In some settings infants are tested for their capacity for nutritive suckling, or they receive structured training in sucking on a gloved finger before breastfeeding is introduced. However, these interventions result in unjustified delays in the introduction of breastfeeding.
8. Preterm infants are more active at the breast when they are held with still caregiver hands; stroking and/or tickling are too stimulating for these little warriors during feeds.
9. Feeding at breast with an SNS if infant is required to receive any form of supplementation can help stimulate milk supply, promote breastfeeding, and ensure the infant is getting the volume of fortified feed they need while still making it possible for infant to feed directly at breast.
10. Cup feeding or finger feeding are also alternatives if infant requires supplementation.
Paced bottle feeds can help to reduce infant fatigue, decrease negative impacts on breastfeeding, and help infant to develop stronger sucking skills as well as endurance needed for breastfeeding.
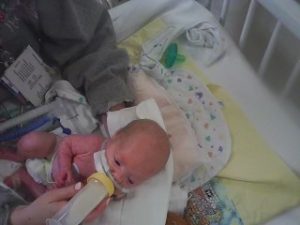
Remember breastfeeding is not all or nothing! Any breastmilk a Mom is able to provide, regardless of how it’s fed, is beneficial to baby.
Transitioning baby exclusively to breast may not happen prior to being discharged home. Connect with a Lactation Consultant early on and develop a plan!

Brittany Chowdhary, RN, CLC, IBCLC
Lactation Consultant Specialist
e || [email protected]
p || (419)872-2255












